Performed by Dr. Apurva Patel, Hip Replacement Surgeon in Ahmedabad
Patient’s Problem
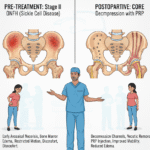
Mrs. Nishi(Name changed for Privacy), a 26-year-old patient living with sickle cell disease, presented with progressively worsening hip pain for more than two years. The pain severely restricted her ability to walk, stand, or sit, and her leg had become shorter due to femoral head collapse and hip deformity. Her condition and pain level (VAS 7–8) made her fear losing mobility at a very young age.
This case aligns closely with findings in the research study, where most patients were young adults in the second to third decades of life, often presenting late with advanced-stage hip damage.
Diagnosis
Clinical evaluation and radiographic assessment confirmed:
- Advanced Avascular Necrosis (AVN) – Modified Ficat–Arlet Stage III–IV
- Collapse of the femoral head
- Fixed flexion & adduction deformities
- Leg shortening (1–3 cm)
- High pain score (VAS 7–8)
- Low Harris Hip Score (~49)
These findings are consistent with the study cohort’s pre-operative characteristics, where the mean Harris Hip Score was 49.75, and most patients presented with advanced (stage IV) AVN and deformities.
Because the disease had progressed beyond the point where medications or decompression could help, the recommended treatment was Total Hip Arthroplasty (THA).
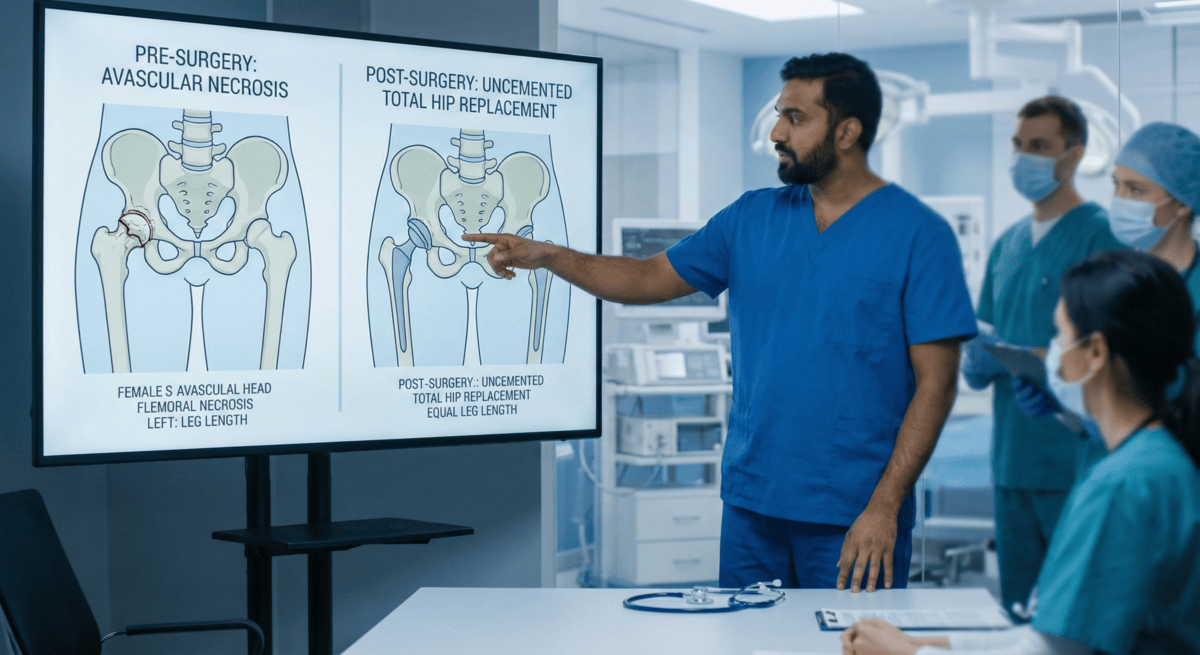
Treatment: Uncemented Total Hip Arthroplasty
The treatment plan followed scientific guidelines outlined in the research study. The surgery was performed by an experienced orthopedic arthroplasty team.
Doctors Involved & Their Roles
- Dr. Arvindkumar — Professor, Department of Orthopaedics, PIMSR (Corresponding Author)
- Senior member of the arthroplasty team
- Guided surgical protocol, implant planning, and postoperative evaluation
- Oversaw research design and clinical methodology
- Dr. Apurva Patel — Senior Resident, Department of Orthopaedics, PIMSR
- Performed Uncemented Total Hip Arthroplasty
- Responsible for surgical execution using the posterior Moore’s approach
- Managed intraoperative challenges and implant positioning
- Dr. Smit Vadher — Consultant Orthopedic Surgeon, HCG Hospital
- Contributed to surgical planning and patient selection criteria
- Part of the operative and postoperative monitoring team
- Dr. Chiragkumar Ninama — Junior Resident, Orthopaedics, PIMSR
- Assisted intraoperatively
- Managed preoperative templating, patient preparation, and immediate post-op rehabilitation
- Dr. Virag Shah — Junior Resident, Orthopaedics, PIMSR
- Assisted with postoperative physiotherapy protocols
- Participated in follow-up assessments & data collection
- Dr. Sonal Lakum — Assistant Professor, Department of Microbiology
- Managed infection prevention, microbiological assessments, and culture analysis for infections
- Played a key role in managing postoperative wound infection protocols
Surgical Method
- Thorough pre-operative templating for correct implant sizing, stem position, cup inclination, and limb length restoration
- Posterior Moore’s approach, as used in all 20 hips in the research study
- Uncemented implants are preferred due to better long-term fixation in young patients with sickle cell disease
- Prophylactic antibiotics before incision
- Drain removal on POD-2
- Infection control precautions, crucial in sickle cell patients
- Early physiotherapy from Day 1
- Toe-touch to full weight-bearing progression within the first 1–2 weeks
This protocol mirrors the exact steps used across all surgeries in the research dataset.
Outcome: Before-and-After Transformation
Before Surgery
- Severe hip pain
- Difficulty walking
- Leg shortening
- Progressive deformity
- VAS 7–8
- Harris Hip Score: ~49
- Fear of disability
These symptoms are consistent with the preoperative profile of most patients in the study.
After Surgery
- Complete relief from hip pain (mean VAS reduced from 7.8 to 0.78)
- Restored walking pattern
- Leg length equalization / minimal residual discrepancy
- No postoperative deformity
- Return to work within ~3 months
- Harris Hip Score improved from 49.75 to 87.3
- Significant gait improvement
These reflect the study’s outcomes, where:
- 60% had excellent results
- 15% had good results
- 20% had fair results
- 5% had poor results (mostly due to infection or sciatic nerve injury)
Mrs. Nishi fell into the category of excellent postoperative outcome.
Conclusion
This case demonstrates how Uncemented Total Hip Arthroplasty provides transformative results for patients with advanced Avascular Necrosis associated with sickle cell disease.
The research proves that, even with the complexity of sickle cell hemoglobinopathy, THA can deliver:
- Reliable pain relief
- Increased mobility
- Improved limb alignment
- High patient satisfaction
- Predictable functional outcomes
Thanks to a skilled multidisciplinary team including
Dr. Arvindkumar, Dr. Apurva Patel, Dr. Smit Vadher, Dr. Chiragkumar Ninama, Dr. Virag Shah, and Dr. Sonal Lakum patients can achieve a pain-free and active lifestyle again.